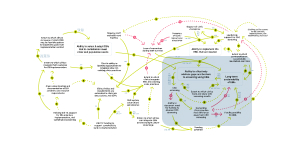
How does CRC screening impact EBI sustainability?
At the center of this CLD are two balancing loops. Balancing loop 1 starts with increasing the long-term sustainability of EBIs, which in turn increases a clinic’s ability to effectively address gaps and barriers to screening using EBIs,139 and boosts CRC screening.75, 201, 305, 332, 354, 407, 445 This, in turn, enhances the long-term sustainability of EBIs.
However, after a clinic achieves high CRC screening rates, their priorities may shift away from improving CRC screening,266 reducing the focus on CRC screening and decreasing the long-term sustainability of EBIs.126, 153 This completes balancing loop 2. Similarly, a higher number of competing clinic priorities makes it more likely that funding will be allocated elsewhere,153 further reducing EBI sustainability.114, 127, 155
Finally, the extent to which clinics track and share CRC screening results impacts both the sustainability of EBIs and their effective use. Tracking results enables clinics to evaluate EBI performance and make improvements to enhance screening.107, 327, 440 Balancing loops 1 and 2 together form the basis of balancing loop 3, which is described below.
Cited references for this diagram
Studying factors associated with maintaining or abandoning the EBIs will create a catalog of lessons learned that can be shared among grantees to help them increase effectiveness in selecting and implementing EBIs.
Hannon PA, Maxwell AE, Escoffery C, Vu T, Kohn M, Leeman J, Carvalho ML, Pfeiffer DJ, Dwyer A, Fernandez ME, Vernon SW, Liang L, DeGroff A. Colorectal Cancer Control Program grantees' use of evidence-based interventions. Am J Prev Med. 2013 Nov;45(5):644-8. doi: 10.1016/j.amepre.2013.06.010. PMID: 24139779; PMCID: PMC4618374.
Other frequently mentioned barriers [to EBI implementation] included getting approvals or arranging contracts with partner agencies and concerns about funding and sustainability.
Hannon PA, Maxwell AE, Escoffery C, Vu T, Kohn MJ, Gressard L, Dillon-Sumner L, Mason C, DeGroff A. Adoption and Implementation of Evidence-Based Colorectal Cancer Screening Interventions Among Cancer Control Program Grantees, 2009-2015. Prev Chronic Dis. 2019 Oct 10;16:E139. doi: 10.5888/pcd16.180682. PMID: 31603404; PMCID: PMC6795067.
A couple of grantees also noted a shift in their partners’ focus or priorities that led to the partner no longer being interested in the EBI.
Hannon PA, Maxwell AE, Escoffery C, Vu T, Kohn MJ, Gressard L, Dillon-Sumner L, Mason C, DeGroff A. Adoption and Implementation of Evidence-Based Colorectal Cancer Screening Interventions Among Cancer Control Program Grantees, 2009-2015. Prev Chronic Dis. 2019 Oct 10;16:E139. doi: 10.5888/pcd16.180682. PMID: 31603404; PMCID: PMC6795067.
Few grantees provided reasons for discontinuing specific EBIs. Of those who did, a common reason given (especially in program year 6) was the end of funding to sustain the EBI.
Hannon PA, Maxwell AE, Escoffery C, Vu T, Kohn MJ, Gressard L, Dillon-Sumner L, Mason C, DeGroff A. Adoption and Implementation of Evidence-Based Colorectal Cancer Screening Interventions Among Cancer Control Program Grantees, 2009-2015. Prev Chronic Dis. 2019 Oct 10;16:E139. doi: 10.5888/pcd16.180682. PMID: 31603404; PMCID: PMC6795067.
Implementation readiness — an organization’s combined capacity, commitment, and willingness to implement a new program, policy, or practice — facilitates implementation success.[[16–18]] Because public health resources are limited, identifying a clinic’s readiness to successfully implement and sustain interventions, as well as gaps in clinic resources or practices that need to be addressed before implementation, is critical. Such assessment practices can guide clinics to select interventions with the greatest potential for long-term sustainability, and in turn help maximize the impact of public health spending, optimize clinic success, reduce cancer disparities, and improve population health.
Hohl SD, Melillo S, Vu TT, Escoffery C, DeGroff A, Schlueter D, Ross LW, Maxwell AE, Sharma KP, Boehm J, Joseph D, Hannon PA. Development of a Field Guide for Assessing Readiness to Implement Evidence-Based Cancer Screening Interventions in Primary Care Clinics. Prev Chronic Dis. 2022 May 12;19:E25. doi: 10.5888/pcd19.210395. PMID: 35550244; PMCID: PMC9109642.
Only 58% of clinics reported having good leadership support to maintain implementation of CRC screening EBIs, including mailed fecal testing. Fewer clinics reported having funding stability, organizational capacity, or the ability to adapt practices to ensure sustainability of EBI implementation. Although the CRCCP and other programs are designed with sustainability as a long-term goal, sustainability is an on-going challenge in clinics with limited resources and changing priorities that are reflected in budget changes.
Hohl SD, Maxwell AE, Sharma KP, Sun J, Vu TT, DeGroff A, Escoffery C, Schlueter D, Hannon PA. Implementing Mailed Colorectal Cancer Fecal Screening Tests in Real-World Primary Care Settings: Promising Implementation Practices and Opportunities for Improvement. Prev Sci. 2024 Apr;25(Suppl 1):124-135. doi: 10.1007/s11121-023-01496-3. Epub 2023 Mar 23. PMID: 36952143; PMCID: PMC10034905.
Over half of clinics (58%) reported having leadership support to a great/very great extent to sustain the implementation of EBIs after the CRCCP screening initiative ends, but only 29% reported having a great/very great extent of funding stability in place to do so (Table 7).
Hohl SD, Maxwell AE, Sharma KP, Sun J, Vu TT, DeGroff A, Escoffery C, Schlueter D, Hannon PA. Implementing Mailed Colorectal Cancer Fecal Screening Tests in Real-World Primary Care Settings: Promising Implementation Practices and Opportunities for Improvement. Prev Sci. 2024 Apr;25(Suppl 1):124-135. doi: 10.1007/s11121-023-01496-3. Epub 2023 Mar 23. PMID: 36952143; PMCID: PMC10034905.
Third, the effectiveness of these EBIs on CRC order and screening uptake was significant across all populations served and independent of insurance status.
Kim KE, Tangka FKL, Jayaprakash M, Randal FT, Lam H, Freedman D, Carrier LA, Sargant C, Maene C, Hoover S, Joseph D, French C, Subramanian S. Effectiveness and Cost of Implementing Evidence-Based Interventions to Increase Colorectal Cancer Screening Among an Underserved Population in Chicago. Health Promot Pract. 2020 Nov;21(6):884-890. doi: 10.1177/1524839920954162. Epub 2020 Sep 29. PMID: 32990041; PMCID: PMC7894065.
Initial investments may discontinue following short-term improvements to population health outcomes, after which implementation of evidence-based practices can diminish, resulting in loss of preliminary program gains (Birken et al., 2020; Buchanan et al., 2005; Stirman et al., 2012).
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
All four priority EBIs were positively associated with clinic screening rates with statistical significance (Table 3).
Sharma KP, DeGroff A, Scott L, Shrestha S, Melillo S, Sabatino SA. Correlates of colorectal cancer screening rates in primary care clinics serving low income, medically underserved populations. Prev Med. 2019 Sep;126:105774. doi: 10.1016/j.ypmed.2019.105774. Epub 2019 Jul 15. PMID: 31319118; PMCID: PMC6904949.
An earlier study reported a 4.4−percentage point increase in average screening rate after 1 year of CRCCP implementation,10 whereas this study observed an increase of 11.3 percentage points over 2 years. Results from this study suggest increased effectiveness of the EBIs with longer and possibly improved implementation in the second year after the initial start-up phase.
Sharma KP, DeGroff A, Maxwell AE, Cole AM, Escoffery NC, Hannon PA. Evidence-Based Interventions and Colorectal Cancer Screening Rates: The Colorectal Cancer Screening Program, 2015-2017. Am J Prev Med. 2021 Sep;61(3):402-409. doi: 10.1016/j.amepre.2021.03.002. Epub 2021 May 14. PMID: 33994253; PMCID: PMC11008572.
Overall, the average clinic-level screening rate increased by 11.7 percentage points from baseline (33.5%) to PY2 (45.2%).
Sharma KP, DeGroff A, Maxwell AE, Cole AM, Escoffery NC, Hannon PA. Evidence-Based Interventions and Colorectal Cancer Screening Rates: The Colorectal Cancer Screening Program, 2015-2017. Am J Prev Med. 2021 Sep;61(3):402-409. doi: 10.1016/j.amepre.2021.03.002. Epub 2021 May 14. PMID: 33994253; PMCID: PMC11008572.
Average clinic CRC screening rates generally increased when clinics implemented or enhanced any number EBIs or SAs compared to clinics that did not newly implement or enhance any EBIs/SAs.
Sharma KP, DeGroff A, Hohl SD, Maxwell AE, Escoffery NC, Sabatino SA, Joseph DA. Multi-component interventions and change in screening rates in primary care clinics in the Colorectal Cancer Control Program. Prev Med Rep. 2022 Jul 9;29:101904. doi: 10.1016/j.pmedr.2022.101904. PMID: 35864930; PMCID: PMC9294188.
Across all interventions and multicomponent interventions, increases in the overall FQHC screening uptake ranged from 4.9 to 26.7 percentage points. Each FQHC implemented interventions that increased CRC screening among its low-income population.
Subramanian S, Tangka FKL, Hoover S. Role of an Implementation Economics Analysis in Providing the Evidence Base for Increasing Colorectal Cancer Screening. Prev Chronic Dis. 2020 Jun 25;17:E46. doi: 10.5888/pcd17.190407. PMID: 32584756; PMCID: PMC7316416.
Implementation sites often differ in the types and combination of EBI(s) and SA(s) implemented, how the EBI(s) and SA(s) are implemented, and the amount of resources utilized for development and implementation. Therefore, comparison across programs should include an in-depth description or mapping of intervention processes to understand how programs are similar and how they differ to support future implementation efforts.
Tangka FKL, Subramanian S, Hoover S, Lara C, Eastman C, Glaze B, Conn ME, DeGroff A, Wong FL, Richardson LC. Identifying optimal approaches to scale up colorectal cancer screening: an overview of the centers for disease control and prevention (CDC)'s learning laboratory. Cancer Causes Control. 2019 Feb;30(2):169-175. doi: 10.1007/s10552-018-1109-x. Epub 2018 Dec 14. PMID: 30552592; PMCID: PMC6382575.
Screening uptake increased across all the sites during the implementation period, ranging from 7.1 to 18.9 % points.
Tangka FKL, Subramanian S, Hoover S, Lara C, Eastman C, Glaze B, Conn ME, DeGroff A, Wong FL, Richardson LC. Identifying optimal approaches to scale up colorectal cancer screening: an overview of the centers for disease control and prevention (CDC)'s learning laboratory. Cancer Causes Control. 2019 Feb;30(2):169-175. doi: 10.1007/s10552-018-1109-x. Epub 2018 Dec 14. PMID: 30552592; PMCID: PMC6382575.
Early results from our PY1 evaluation, including changes in screening rates, suggest the CRCCP is working; program reach was measurable and substantial, clinics enhanced EBIs in place or implemented new ones in clinics, and we observed an increase in the overall average screening rate.
DeGroff A, Sharma K, Satsangi A, Kenney K, Joseph D, Ross K, Leadbetter S, Helsel W, Kammerer W, Firth R, Rockwell T, Short W, Tangka F, Wong F, Richardson L. Increasing Colorectal Cancer Screening in Health Care Systems Using Evidence-Based Interventions. Prev Chronic Dis. 2018 Aug 9;15:E100. doi: 10.5888/pcd15.180029. PMID: 30095405; PMCID: PMC6093266.