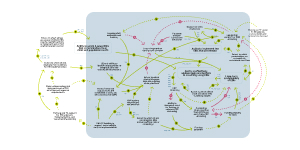
How can sustainability be considered in the early phases of EBI implementation?
This part of the CLD focuses on how sustainability can be considered in the early phases of EBI implementation. One example of this is using CRCCP funding for EHR system automation/optimization,215, 251, 311 which allows EBIs like patient and provider reminders to be incorporated easily into existing clinic practices.71, 115 Similarly, it allows clinics to integrate EBIs across multiple cancer screenings by improving data sharing.356, 360-362
Increasing the extent to which clinics integrate EBIs across multiple cancer screenings and the extent to which they integrate EBIs into existing clinic practices216, 245, 271 are two ways to promote EBI sustainability. Another benefit of integrating EBIs across cancer screenings is that it increases the funding potential of the EBIs because multiple funding streams can be combined.249, 359
Providing ongoing staff education and training in addition to the integration of EBIs into existing clinic practices minimizes the loss of momentum for CRC screening due to staff turnover. Long-term sustainability of EBIs is realized when the loss of momentum for CRC screening due to staff turnover is limited.111, 411
Cited references for this diagram
The other most commonly given reasons for stopping specific EBIs included limited staff time or staff turnover and the desire to implement other EBIs (and not being able to implement all EBIs at one time).
Hannon PA, Maxwell AE, Escoffery C, Vu T, Kohn MJ, Gressard L, Dillon-Sumner L, Mason C, DeGroff A. Adoption and Implementation of Evidence-Based Colorectal Cancer Screening Interventions Among Cancer Control Program Grantees, 2009-2015. Prev Chronic Dis. 2019 Oct 10;16:E139. doi: 10.5888/pcd16.180682. PMID: 31603404; PMCID: PMC6795067.
We found that grantees’ reasons for discontinuing an EBI most often related to capacity issues. Context also may be an important factor. For instance, electronic health records systems were identified as a barrier to EBI implementation. This suggests that sustainability in clinic settings may be challenged when electronic health records systems cannot support integration of client and provider reminder systems as well as provider assessment and feedback reports.
Hannon PA, Maxwell AE, Escoffery C, Vu T, Kohn MJ, Gressard L, Dillon-Sumner L, Mason C, DeGroff A. Adoption and Implementation of Evidence-Based Colorectal Cancer Screening Interventions Among Cancer Control Program Grantees, 2009-2015. Prev Chronic Dis. 2019 Oct 10;16:E139. doi: 10.5888/pcd16.180682. PMID: 31603404; PMCID: PMC6795067.
Uptake may be facilitated through technical and financial support provided by CRCCP awardees and integration of these strategies into clinic electronic health records systems.
Maxwell AE, DeGroff A, Hohl SD, Sharma KP, Sun J, Escoffery C, Hannon PA. Evaluating Uptake of Evidence-Based Interventions in 355 Clinics Partnering With the Colorectal Cancer Control Program, 2015-2018. Prev Chronic Dis. 2022 May 19;19:E26. doi: 10.5888/pcd19.210258. PMID: 35588522; PMCID: PMC9165474.
Among clinics that had EBIs and SAs in place by the end of each year, most considered those EBIs and SAs fully integrated into health systems or clinic operations and sustainable with or without CRCCP resources, especially in years 2 and 3 (Table 4).
Maxwell AE, DeGroff A, Hohl SD, Sharma KP, Sun J, Escoffery C, Hannon PA. Evaluating Uptake of Evidence-Based Interventions in 355 Clinics Partnering With the Colorectal Cancer Control Program, 2015-2018. Prev Chronic Dis. 2022 May 19;19:E26. doi: 10.5888/pcd19.210258. PMID: 35588522; PMCID: PMC9165474.
Given the limited nature of public health funding cycles, it is critical that health systems change efforts not only work to achieve population health outcomes but also dedicate time and resources to integrating effective strategies for increased likelihood of long-term sustainability. Integrating EBIs and SAs into existing FQHC processes proved essential to CRCCP sustainability.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
Respondents across all four awardees discussed integration as a way to expand patient reach across chronic disease programs; decrease staff and patient burden; and support sustainability by pooling implementation resources for increased efficiency.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
Respondents noted the importance of planning for sustainability from initiation of CRCCP implementation by allocating funding to integrate EBIs into FQHC practices. Respondents reported that FQHCs were encouraged to apply funding in ways that directly supported sustainability, such as building infrastructure and long-term FQHC practices (e.g., EHR assessments, quality improvement [QI] efforts, and workflow adaptations) versus funding staff positions (e.g., patient navigators) requiring new funding sources once CRCCP funding ends.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
A key theme across all awardees was the essential nature of coordinating EBIs and SAs with existing FQHC practices to expand reach of clinics’ prevention efforts and increase efficiency.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
This most recent study adds further support to the analysis by the Community Preventive Services Task Force demonstrating that multicomponent interventions led to greater increases in CRC screening.[[13]] Increasing the number of EBIs may be accomplished through the integration of some EBIs such as provider reminders, patient reminders, and provider assessment and feedback into electronic health record systems. Although an upfront investment of time and resources may be needed to accomplish this, resource needs would then diminish, and the sustainability of the EBIs would be enhanced.
Sharma KP, Leadbetter S, DeGroff A. Characterizing clinics with differential changes in the screening rate in the Colorectal Cancer Control Program of the Centers for Disease Control and Prevention. Cancer. 2021 Apr 1;127(7):1049-1056. doi: 10.1002/cncr.33325. Epub 2020 Dec 10. PMID: 33301173; PMCID: PMC9242539.
EHR systems, a reservoir of patient information, were also found to be an important component of information sharing to support integrated implementation. Although investing in functional EHR systems can be costly, these systems are recognized as essential to enable optimal, integrated, patient-centered care because they allow for the abstraction of accurate clinical information.
Soloe C, Arena L, Schlueter D, Melillo S, DeGroff A, Tangka F, Hoover S, Subramanian S. Factors that support readiness to implement integrated evidence-based practice to increase cancer screening. Implement Sci Commun. 2022 Oct 6;3(1):106. doi: 10.1186/s43058-022-00347-6. PMID: 36199117; PMCID: PMC9535984.
We found that readiness for integration in clinics was supported when programs consolidated funding into single contracts for partner clinics, rather than providing separate “siloed” contracts for individual health conditions. In the CRCCP, this approach presents an opportunity for more efficient use of public health funding for coordinated promotion of cancer screenings (e.g., colorectal, breast, and/or cervical). Efficiencies are also achieved when the clinic staff respond to a single, consolidated funding application rather than multiple applications, and the pooled funding provides both program sites and clinic flexibility to leverage funds and share overhead costs, offering the opportunity to achieve more with their awarded funds.
Soloe C, Arena L, Schlueter D, Melillo S, DeGroff A, Tangka F, Hoover S, Subramanian S. Factors that support readiness to implement integrated evidence-based practice to increase cancer screening. Implement Sci Commun. 2022 Oct 6;3(1):106. doi: 10.1186/s43058-022-00347-6. PMID: 36199117; PMCID: PMC9535984.
The ability to access and share accurate patient information, including EHR data, was identified as another factor supporting readiness for integrated implementation of CRC screening.
Soloe C, Arena L, Schlueter D, Melillo S, DeGroff A, Tangka F, Hoover S, Subramanian S. Factors that support readiness to implement integrated evidence-based practice to increase cancer screening. Implement Sci Commun. 2022 Oct 6;3(1):106. doi: 10.1186/s43058-022-00347-6. PMID: 36199117; PMCID: PMC9535984.
Participants indicated that the clinic staff, particularly patient navigators and care coordinators, rely on the availability of accurate EHR reports to identify patients for screening and/or diagnostics for multiple chronic disease conditions. The clinic staff emphasized that the utility of the EHR data in supporting integrated implementation is contingent on data accuracy.
Soloe C, Arena L, Schlueter D, Melillo S, DeGroff A, Tangka F, Hoover S, Subramanian S. Factors that support readiness to implement integrated evidence-based practice to increase cancer screening. Implement Sci Commun. 2022 Oct 6;3(1):106. doi: 10.1186/s43058-022-00347-6. PMID: 36199117; PMCID: PMC9535984.
Similarly, data sharing among quality improvement (QI) teams promotes a collective understanding of where clinics stand on the delivery of health promotion activities that can foster understanding of opportunities to potentially improve these metrics through integrated implementation.
Soloe C, Arena L, Schlueter D, Melillo S, DeGroff A, Tangka F, Hoover S, Subramanian S. Factors that support readiness to implement integrated evidence-based practice to increase cancer screening. Implement Sci Commun. 2022 Oct 6;3(1):106. doi: 10.1186/s43058-022-00347-6. PMID: 36199117; PMCID: PMC9535984.
Third, staff turnover was seen as a major barrier to both implementation success and sustainability. The burden consists of the need to train new staff, the loss of institutional knowledge, and the need to rebuild informal communication channels that are often required for coordination of multilevel interventions and supporting activities.
Subramanian S, Tangka FKL, Hoover S, DeGroff A. Integrated interventions and supporting activities to increase uptake of multiple cancer screenings: conceptual framework, determinants of implementation success, measurement challenges, and research priorities. Implement Sci Commun. 2022 Oct 5;3(1):105. doi: 10.1186/s43058-022-00353-8. PMID: 36199098; PMCID: PMC9532830.
However, less than 50% of clinics used CRCCP resources for provider reminders in PY1. Provider reminders can increase screening rates by a median of 15.3%.[[24]] If reminders are integrated into an electronic health system, the activity is sustainable.
DeGroff A, Sharma K, Satsangi A, Kenney K, Joseph D, Ross K, Leadbetter S, Helsel W, Kammerer W, Firth R, Rockwell T, Short W, Tangka F, Wong F, Richardson L. Increasing Colorectal Cancer Screening in Health Care Systems Using Evidence-Based Interventions. Prev Chronic Dis. 2018 Aug 9;15:E100. doi: 10.5888/pcd15.180029. PMID: 30095405; PMCID: PMC6093266.