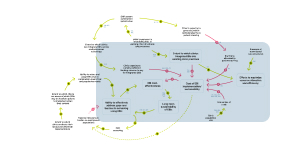
What factors impact the cost of implementation and sustainability?
The focal point of this diagram is the cost of EBI implementation and sustainability and how it relates to EBI cost-effectiveness (i.e., the value per dollar spent). Both the extent to which clinics integrate EBIs into existing clinic practices212, 245 and their efforts to maximize resources175 inversely relate to the cost of EBI implementation and sustainability. Decreasing the cost of EBI implementation and sustainability increases its cost-effectiveness.
A reinforcing loop (R1) exists because increasing the cost-effectiveness of an EBI enhances its sustainability139, 245, 311 since it requires fewer resources over time. This increases the clinic’s ability to effectively address gaps and barriers to screening using EBIs.139, 153, 245 When clinics successfully address these screening gaps, the EBIs used become more cost-effective due to increasing the number of individuals who are up to date on CRC screening.175
Cited references for this diagram
Implementation readiness — an organization’s combined capacity, commitment, and willingness to implement a new program, policy, or practice — facilitates implementation success.[[16–18]] Because public health resources are limited, identifying a clinic’s readiness to successfully implement and sustain interventions, as well as gaps in clinic resources or practices that need to be addressed before implementation, is critical. Such assessment practices can guide clinics to select interventions with the greatest potential for long-term sustainability, and in turn help maximize the impact of public health spending, optimize clinic success, reduce cancer disparities, and improve population health.
Hohl SD, Melillo S, Vu TT, Escoffery C, DeGroff A, Schlueter D, Ross LW, Maxwell AE, Sharma KP, Boehm J, Joseph D, Hannon PA. Development of a Field Guide for Assessing Readiness to Implement Evidence-Based Cancer Screening Interventions in Primary Care Clinics. Prev Chronic Dis. 2022 May 12;19:E25. doi: 10.5888/pcd19.210395. PMID: 35550244; PMCID: PMC9109642.
Only 58% of clinics reported having good leadership support to maintain implementation of CRC screening EBIs, including mailed fecal testing. Fewer clinics reported having funding stability, organizational capacity, or the ability to adapt practices to ensure sustainability of EBI implementation. Although the CRCCP and other programs are designed with sustainability as a long-term goal, sustainability is an on-going challenge in clinics with limited resources and changing priorities that are reflected in budget changes.
Hohl SD, Maxwell AE, Sharma KP, Sun J, Vu TT, DeGroff A, Escoffery C, Schlueter D, Hannon PA. Implementing Mailed Colorectal Cancer Fecal Screening Tests in Real-World Primary Care Settings: Promising Implementation Practices and Opportunities for Improvement. Prev Sci. 2024 Apr;25(Suppl 1):124-135. doi: 10.1007/s11121-023-01496-3. Epub 2023 Mar 23. PMID: 36952143; PMCID: PMC10034905.
Program planners should carefully consider the potential reach and infrastructure costs of direct CRC screening services given available sources of funding, the size of the potential target population relative to the capacity and funding of program implementers, the selection of EBIs that maximize program effects while minimizing costs, and the ability of program implementers to leverage the resources of other public and nonpublic health organizations to facilitate implementation.
Joseph DA, DeGroff A. The CDC Colorectal Cancer Control Program, 2009-2015. Prev Chronic Dis. 2019 Dec 5;16:E159. doi: 10.5888/pcd16.190336. PMID: 31808418; PMCID: PMC6896829.
Another explanation is that some EBIs and SAs can be integrated into clinical practice through clinics’ electronic health records systems. For example, by using data from electronic health records, patient reminder letters can be generated and personalized with each patient’s name and address, preferred language, the name of the patient’s primary care provider, and their history of CRC screening (eg, type and time of most recent test). Although it takes resources to program electronic health records and to set up these strategies initially, clinic health information technology and automated calling and texting systems can support implementation.[[27,28]]
Maxwell AE, DeGroff A, Hohl SD, Sharma KP, Sun J, Escoffery C, Hannon PA. Evaluating Uptake of Evidence-Based Interventions in 355 Clinics Partnering With the Colorectal Cancer Control Program, 2015-2018. Prev Chronic Dis. 2022 May 19;19:E26. doi: 10.5888/pcd19.210258. PMID: 35588522; PMCID: PMC9165474.
Given the limited nature of public health funding cycles, it is critical that health systems change efforts not only work to achieve population health outcomes but also dedicate time and resources to integrating effective strategies for increased likelihood of long-term sustainability. Integrating EBIs and SAs into existing FQHC processes proved essential to CRCCP sustainability.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
This most recent study adds further support to the analysis by the Community Preventive Services Task Force demonstrating that multicomponent interventions led to greater increases in CRC screening.[[13]] Increasing the number of EBIs may be accomplished through the integration of some EBIs such as provider reminders, patient reminders, and provider assessment and feedback into electronic health record systems. Although an upfront investment of time and resources may be needed to accomplish this, resource needs would then diminish, and the sustainability of the EBIs would be enhanced.
Sharma KP, Leadbetter S, DeGroff A. Characterizing clinics with differential changes in the screening rate in the Colorectal Cancer Control Program of the Centers for Disease Control and Prevention. Cancer. 2021 Apr 1;127(7):1049-1056. doi: 10.1002/cncr.33325. Epub 2020 Dec 10. PMID: 33301173; PMCID: PMC9242539.