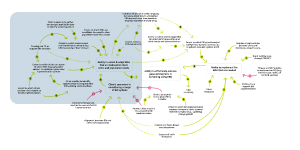
What impacts a clinic's ability to select and adapt EBIs to meet their specific population's needs?
This section of the CLD focuses on factors that impact how well a clinic can select and adapt EBIs to fit their population’s needs. A clinic’s openness to all EBIs directly increases its ability to select and adapt EBIs for their specific context.
Conducting readiness assessments is a crucial step for EBI selection as it allows the clinic to evaluate existing practices and identify opportunities to integrate EBIs.270 It also helps clinics understand which EBIs are feasible to implement given their resources.140, 198-200, 273, 334, 455 Identifying opportunities to integrate EBIs into existing practices improves feasibility and implementation.212, 216, 219 Clinics aware of this feasibility are more likely to select and adapt EBIs for their populations.245, 264, 271, 443
Providing training and TA for EBI selection increases awareness of EBI feasibility and the ability to assess factors impacting screening rates.85, 457 Understanding CRC screening threats specific to the clinic’s context enhances their ability to select EBIs that address those threats.435 Training and TA also improve the ability to select and combine EBIs effectively.
The more modifiable an EBI is, the more likely it will be selected and adapted for the clinic’s context.195, 198, 208, 318, 436, 437 Additionally, a clinic’s capacity to gather and analyze population-level data relies on its EHR system.256, 360, 362 A well-functioning EHR system helps identify screening needs and share information across programs.
Cited references for this diagram
Key informants who represented current and previous recipients generally said that mixed-methods assessments conducted before implementation prepared them to use results to inform development of tailored action plans for EBI implementation and technical assistance with partners.
Hohl SD, Melillo S, Vu TT, Escoffery C, DeGroff A, Schlueter D, Ross LW, Maxwell AE, Sharma KP, Boehm J, Joseph D, Hannon PA. Development of a Field Guide for Assessing Readiness to Implement Evidence-Based Cancer Screening Interventions in Primary Care Clinics. Prev Chronic Dis. 2022 May 12;19:E25. doi: 10.5888/pcd19.210395. PMID: 35550244; PMCID: PMC9109642.
Second, each EBI was modified to fit the needs and staffing model for this health system, which may have improved efficiency and impact.
Kim KE, Tangka FKL, Jayaprakash M, Randal FT, Lam H, Freedman D, Carrier LA, Sargant C, Maene C, Hoover S, Joseph D, French C, Subramanian S. Effectiveness and Cost of Implementing Evidence-Based Interventions to Increase Colorectal Cancer Screening Among an Underserved Population in Chicago. Health Promot Pract. 2020 Nov;21(6):884-890. doi: 10.1177/1524839920954162. Epub 2020 Sep 29. PMID: 32990041; PMCID: PMC7894065.
This study demonstrates that EBIs to increase CRC screening may be effective in clinics with fewer resources that serve populations who have poor access to or under-utilize health care services. Tailoring the EBIs to the needs and capacity of participating clinics may have been key to their effectiveness.
Kim KE, Tangka FKL, Jayaprakash M, Randal FT, Lam H, Freedman D, Carrier LA, Sargant C, Maene C, Hoover S, Joseph D, French C, Subramanian S. Effectiveness and Cost of Implementing Evidence-Based Interventions to Increase Colorectal Cancer Screening Among an Underserved Population in Chicago. Health Promot Pract. 2020 Nov;21(6):884-890. doi: 10.1177/1524839920954162. Epub 2020 Sep 29. PMID: 32990041; PMCID: PMC7894065.
Using a participatory implementation approach, a pre-implementation assessment was conducted to assess readiness for implementation of EBIs in order to increase CRC screening uptake.
Kim KE, Tangka FKL, Jayaprakash M, Randal FT, Lam H, Freedman D, Carrier LA, Sargant C, Maene C, Hoover S, Joseph D, French C, Subramanian S. Effectiveness and Cost of Implementing Evidence-Based Interventions to Increase Colorectal Cancer Screening Among an Underserved Population in Chicago. Health Promot Pract. 2020 Nov;21(6):884-890. doi: 10.1177/1524839920954162. Epub 2020 Sep 29. PMID: 32990041; PMCID: PMC7894065.
First, the pre-implementation process allowed the awardee to determine the infrastructure needs and their capacity to implement EBIs.
Kim KE, Tangka FKL, Jayaprakash M, Randal FT, Lam H, Freedman D, Carrier LA, Sargant C, Maene C, Hoover S, Joseph D, French C, Subramanian S. Effectiveness and Cost of Implementing Evidence-Based Interventions to Increase Colorectal Cancer Screening Among an Underserved Population in Chicago. Health Promot Pract. 2020 Nov;21(6):884-890. doi: 10.1177/1524839920954162. Epub 2020 Sep 29. PMID: 32990041; PMCID: PMC7894065.
National programs like CRCCP must balance the desire for a common campaign identity with the need to help state and local agencies customize resources to best serve their local mix of constituents. For example, CRCCP leaders and their partners must choose specific types of small media and client reminders and adapt them for different settings and populations.
Kreuter MW, Garibay LB, Pfeiffer DJ, Morgan JC, Thomas M, Wilson KM, Pieters J, Szczepaniec K, Scott A, Poor TJ. Small media and client reminders for colorectal cancer screening: current use and gap areas in CDC's Colorectal Cancer Control Program. Prev Chronic Dis. 2012;9:E131. doi: 10.5888/pcd9.110317. Epub 2012 Jul 19. PMID: 22814237; PMCID: PMC3469321.
Another explanation is that some EBIs and SAs can be integrated into clinical practice through clinics’ electronic health records systems. For example, by using data from electronic health records, patient reminder letters can be generated and personalized with each patient’s name and address, preferred language, the name of the patient’s primary care provider, and their history of CRC screening (eg, type and time of most recent test). Although it takes resources to program electronic health records and to set up these strategies initially, clinic health information technology and automated calling and texting systems can support implementation.[[27,28]]
Maxwell AE, DeGroff A, Hohl SD, Sharma KP, Sun J, Escoffery C, Hannon PA. Evaluating Uptake of Evidence-Based Interventions in 355 Clinics Partnering With the Colorectal Cancer Control Program, 2015-2018. Prev Chronic Dis. 2022 May 19;19:E26. doi: 10.5888/pcd19.210258. PMID: 35588522; PMCID: PMC9165474.
Among clinics that had EBIs and SAs in place by the end of each year, most considered those EBIs and SAs fully integrated into health systems or clinic operations and sustainable with or without CRCCP resources, especially in years 2 and 3 (Table 4).
Maxwell AE, DeGroff A, Hohl SD, Sharma KP, Sun J, Escoffery C, Hannon PA. Evaluating Uptake of Evidence-Based Interventions in 355 Clinics Partnering With the Colorectal Cancer Control Program, 2015-2018. Prev Chronic Dis. 2022 May 19;19:E26. doi: 10.5888/pcd19.210258. PMID: 35588522; PMCID: PMC9165474.
Sustainability and integration into clinic operations during the 3-year period increased most for activities that largely focused on providers, such as provider reminder systems, an increase of 14 percentage points from 79% in year 1 to 93% in year 3. Similarly, full integration of provider assessment and feedback increased 27 percentage points, from 69% to 96% of clinics; full integration of professional development or provider education increased by 16 percentage points, from 76% to 92% of clinics, followed by full integration of small media for an increase of 11 percentage points from 81% to 92% of clinics.
Maxwell AE, DeGroff A, Hohl SD, Sharma KP, Sun J, Escoffery C, Hannon PA. Evaluating Uptake of Evidence-Based Interventions in 355 Clinics Partnering With the Colorectal Cancer Control Program, 2015-2018. Prev Chronic Dis. 2022 May 19;19:E26. doi: 10.5888/pcd19.210258. PMID: 35588522; PMCID: PMC9165474.
Given the limited nature of public health funding cycles, it is critical that health systems change efforts not only work to achieve population health outcomes but also dedicate time and resources to integrating effective strategies for increased likelihood of long-term sustainability. Integrating EBIs and SAs into existing FQHC processes proved essential to CRCCP sustainability.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
Effective EHR use is foundational for institutionalizing EBIs and SAs and supports high-quality data management and reporting, thereby making continued implementation more feasible.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
Integrating evidence-based processes into multiple aspects of clinic operations—including funding allocation, staff training, care delivery models, and EHR systems—can be complex but improve the prospect of sustainability.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
Our findings highlight the essential role of awardees in using readiness assessment findings to “meet clinics where they are” and mobilize strength-based partnerships—a critical tenet of public health service—to identify opportunities to integrate EBIs and SAs into existing clinic protocols.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
A key theme across all awardees was the essential nature of coordinating EBIs and SAs with existing FQHC practices to expand reach of clinics’ prevention efforts and increase efficiency.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
Respondents from three awardees described working with FQHCs to formally assess their implementation readiness during the application process or initial site visits. Although the scope of assessments and definitions of “readiness” varied, awardees generally examined: (a) CRC burden and risk, (b) CRC screening practices, (c) experience implementing similar EBIs and SAs, (d) effectively engaging partners, (e) current EHR systems, including problems with EHRs related to EBI implementation or measuring CRC screening rates, and (f) CRC screening rates. FQHC staff, in collaboration with awardees, used assessment results to inform selection of EBIs and SAs for implementation and address EHR issues.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
The EBIs used in the CRCCP can be implemented differently, and practitioners can benefit from ensuring that the interventions are appropriate for their unique clinic population and context.
Sharma KP, Leadbetter S, DeGroff A. Characterizing clinics with differential changes in the screening rate in the Colorectal Cancer Control Program of the Centers for Disease Control and Prevention. Cancer. 2021 Apr 1;127(7):1049-1056. doi: 10.1002/cncr.33325. Epub 2020 Dec 10. PMID: 33301173; PMCID: PMC9242539.
To determine appropriate EBIs and ensure clinic capacity to implement them, programs can conduct readiness assessments of clinics prior to implementation. However, clinics may lack resources to implement all available interventions, and may strategically choose EBIs that are less resource intensive.
Sharma KP, DeGroff A, Hohl SD, Maxwell AE, Escoffery NC, Sabatino SA, Joseph DA. Multi-component interventions and change in screening rates in primary care clinics in the Colorectal Cancer Control Program. Prev Med Rep. 2022 Jul 9;29:101904. doi: 10.1016/j.pmedr.2022.101904. PMID: 35864930; PMCID: PMC9294188.
The ability to access and share accurate patient information, including EHR data, was identified as another factor supporting readiness for integrated implementation of CRC screening.
Soloe C, Arena L, Schlueter D, Melillo S, DeGroff A, Tangka F, Hoover S, Subramanian S. Factors that support readiness to implement integrated evidence-based practice to increase cancer screening. Implement Sci Commun. 2022 Oct 6;3(1):106. doi: 10.1186/s43058-022-00347-6. PMID: 36199117; PMCID: PMC9535984.
Similarly, data sharing among quality improvement (QI) teams promotes a collective understanding of where clinics stand on the delivery of health promotion activities that can foster understanding of opportunities to potentially improve these metrics through integrated implementation.
Soloe C, Arena L, Schlueter D, Melillo S, DeGroff A, Tangka F, Hoover S, Subramanian S. Factors that support readiness to implement integrated evidence-based practice to increase cancer screening. Implement Sci Commun. 2022 Oct 6;3(1):106. doi: 10.1186/s43058-022-00347-6. PMID: 36199117; PMCID: PMC9535984.
Given the large variation across grantees on screening promotion interventions, a systematic assessment of needs matched with promotion activities, and their impact on screening rates, could provide better guidance on optimal resource allocation.
Tangka FKL, Subramanian S, Hoover S, Cole-Beebe M, DeGroff A, Joseph D, Chattopadhyay S. Expenditures on Screening Promotion Activities in CDC's Colorectal Cancer Control Program, 2009-2014. Prev Chronic Dis. 2019 Jun 6;16:E72. doi: 10.5888/pcd16.180337. PMID: 31172915; PMCID: PMC6583814.
Small media was often used at the initiation of the program, and this could be due to the availability of small media materials[[20]] and tools that grantees could easily tailor.
Tangka FKL, Subramanian S, Hoover S, Cole-Beebe M, DeGroff A, Joseph D, Chattopadhyay S. Expenditures on Screening Promotion Activities in CDC's Colorectal Cancer Control Program, 2009-2014. Prev Chronic Dis. 2019 Jun 6;16:E72. doi: 10.5888/pcd16.180337. PMID: 31172915; PMCID: PMC6583814.
Across the 5 years, grantees allocated more resources to small media in the first year of the program. Small media might be easier to implement while other interventions might require more planning; CDC and other organizations provide small media materials that grantees can easily tailor to implement targeted campaigns.
Tangka FKL, Subramanian S, Hoover S, Cole-Beebe M, DeGroff A, Joseph D, Chattopadhyay S. Expenditures on Screening Promotion Activities in CDC's Colorectal Cancer Control Program, 2009-2014. Prev Chronic Dis. 2019 Jun 6;16:E72. doi: 10.5888/pcd16.180337. PMID: 31172915; PMCID: PMC6583814.
Integrating CRC interventions into the standard operating procedures and work flow processes of health systems, when possible, will contribute to sustainability (e.g., incorporating client reminders into the electronic health record system so that reminders are automated).
Tangka FKL, Subramanian S, Hoover S, Lara C, Eastman C, Glaze B, Conn ME, DeGroff A, Wong FL, Richardson LC. Identifying optimal approaches to scale up colorectal cancer screening: an overview of the centers for disease control and prevention (CDC)'s learning laboratory. Cancer Causes Control. 2019 Feb;30(2):169-175. doi: 10.1007/s10552-018-1109-x. Epub 2018 Dec 14. PMID: 30552592; PMCID: PMC6382575.
According to ID-DHW stakeholders, there were several program elements that facilitated the initiation of cancer screening prevention integration after their planning phase. The first of these elements was a pre-implementation checklist for health clinics to determine their capacity for implementing each type of cancer screening and undertake specific enhancements for coordinated and integrated screenings to be initiated.
Tangka FKL, Subramanian S, Hoover S, Cariou C, Creighton B, Hobbs L, Marzano A, Marcotte A, Norton DD, Kelly-Flis P, Leypoldt M, Larkins T, Poole M, Boehm J. Improving the efficiency of integrated cancer screening delivery across multiple cancers: case studies from Idaho, Rhode Island, and Nebraska. Implement Sci Commun. 2022 Dec 16;3(1):133. doi: 10.1186/s43058-022-00381-4. PMID: 36527147; PMCID: PMC9756516.
Grantees also reported a moderate need for training regarding many aspects of EBI implementation, from identifying EBIs and assessing organizational capacity to implement selected EBIs to conducting a process and outcome evaluation.
Escoffery C, Hannon P, Maxwell AE, Vu T, Leeman J, Dwyer A, Mason C, Sowles S, Rice K, Gressard L. Assessment of training and technical assistance needs of Colorectal Cancer Control Program Grantees in the U.S. BMC Public Health. 2015 Jan 31;15:49. doi: 10.1186/s12889-015-1386-1. PMID: 25636329; PMCID: PMC4318175.
Individualized TA can provide more in-depth information on how to implement a specific strategy and also address unique contextual factors (e.g., organizational systems such as paper records or electronic medical records, staffing, resources). These combinations of prevention support reported by grantees match the common strategies found in other studies that promote the adoption of EBIs such as in person training and TA,[[29,30]] packaged materials or recommendations, [[31,32]] and conference calls.[[33]] These prevention supports have been proven to increase adoptions of evidence-based prevention strategies.[[31,32,34]]
Escoffery C, Hannon P, Maxwell AE, Vu T, Leeman J, Dwyer A, Mason C, Sowles S, Rice K, Gressard L. Assessment of training and technical assistance needs of Colorectal Cancer Control Program Grantees in the U.S. BMC Public Health. 2015 Jan 31;15:49. doi: 10.1186/s12889-015-1386-1. PMID: 25636329; PMCID: PMC4318175.