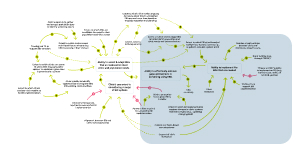
What impacts a clinic's ability to implement the needed EBIs?
Multiple factors support a clinic’s ability to implement EBIs needed for their specific context. Increasing grant funding175, 215 and clinic resources296, 324 enhances EBI implementation. Support from clinic champions260, 262, 314, 326 and training and TA also improve implementation.80-82, 85, 257
A higher number of partnerships between clinics and community organizations,118 as well as the presence of team-based care structures, also strengthens a clinic’s EBI implementation capacity.259, 364 Increasing the extent to which EBIs address multilevel success factors further improves implementation.203
Finally, threats like staff turnover and EHR challenges reduce successful EBI implementation.257, 411, 414
Cited references for this diagram
Across EBIs, many grantees mentioned successful partnerships as key facilitators to implementation. In many cases, grantees’ partners led implementation activities; in others, they provided connections, materials, or staff time.
Hannon PA, Maxwell AE, Escoffery C, Vu T, Kohn MJ, Gressard L, Dillon-Sumner L, Mason C, DeGroff A. Adoption and Implementation of Evidence-Based Colorectal Cancer Screening Interventions Among Cancer Control Program Grantees, 2009-2015. Prev Chronic Dis. 2019 Oct 10;16:E139. doi: 10.5888/pcd16.180682. PMID: 31603404; PMCID: PMC6795067.
Program planners should carefully consider the potential reach and infrastructure costs of direct CRC screening services given available sources of funding, the size of the potential target population relative to the capacity and funding of program implementers, the selection of EBIs that maximize program effects while minimizing costs, and the ability of program implementers to leverage the resources of other public and nonpublic health organizations to facilitate implementation.
Joseph DA, DeGroff A. The CDC Colorectal Cancer Control Program, 2009-2015. Prev Chronic Dis. 2019 Dec 5;16:E159. doi: 10.5888/pcd16.190336. PMID: 31808418; PMCID: PMC6896829.
Findings from these surveys help in understanding and prioritizing the needs of public health agencies and their community partners in implementing evidence-based approaches to increase CRC screening. These needs might best be met by a multilevel approach that includes developing systems to help practice agencies promote long-lasting protective interventions (ie, screening), using effective and audience-specific information and education.[[17]]
Kreuter MW, Garibay LB, Pfeiffer DJ, Morgan JC, Thomas M, Wilson KM, Pieters J, Szczepaniec K, Scott A, Poor TJ. Small media and client reminders for colorectal cancer screening: current use and gap areas in CDC's Colorectal Cancer Control Program. Prev Chronic Dis. 2012;9:E131. doi: 10.5888/pcd9.110317. Epub 2012 Jul 19. PMID: 22814237; PMCID: PMC3469321.
Uptake may be facilitated through technical and financial support provided by CRCCP awardees and integration of these strategies into clinic electronic health records systems.
Maxwell AE, DeGroff A, Hohl SD, Sharma KP, Sun J, Escoffery C, Hannon PA. Evaluating Uptake of Evidence-Based Interventions in 355 Clinics Partnering With the Colorectal Cancer Control Program, 2015-2018. Prev Chronic Dis. 2022 May 19;19:E26. doi: 10.5888/pcd19.210258. PMID: 35588522; PMCID: PMC9165474.
Study results support the need for awardees and implementation partners to provide health systems and clinics with tailored TA for their specific EHR system throughout the funding cycle to support EHR optimization for CRC screening, including avoiding common pitfalls (e.g., improper data entry, overly complex systems, changing EHRs) in ever-changing health care environments.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
Respondents in this study largely discussed the utility of integration within existing team-based care structures. Clinics without team-based structures in place prior to implementing a CRC health systems change effort may require additional support as they adjust to providing integrated services.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
Respondents described aspects of FQHC communication and culture that bolstered early implementation, including the importance of identifying champions from varied roles (e.g., QI expert, physician) during FQHC recruitment or early implementation who could help prioritize CRC screening within FQHCs.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
Whether champions served in leadership or other FQHC staff roles, their ongoing promotion of EBIs and SAs, and clear and consistent leadership support, was paramount to prioritize these efforts. CRC screening champions have been associated with increased CRC screening rates and higher overall clinic performance.
Schlueter D, DeGroff A, Soloe C, Arena L, Melillo S, Tangka F, Hoover S, Subramanian S. Factors That Support Sustainability of Health Systems Change to Increase Colorectal Cancer Screening in Primary Care Clinics: A Longitudinal Qualitative Study. Health Promot Pract. 2023 Jul;24(4):755-763. doi: 10.1177/15248399221091999. Epub 2022 May 18. PMID: 35582930; PMCID: PMC9672135.
That non-FQHC clinics had higher screening rates than FQHCs may highlight the fact that the latter serve patients who are more disadvantaged with lower screening rates than other populations included in this study. Similarly, our finding that clinics with larger patient populations had higher screening rates suggests availability of resources and clinic capacity may underlie their performance.
Sharma KP, DeGroff A, Scott L, Shrestha S, Melillo S, Sabatino SA. Correlates of colorectal cancer screening rates in primary care clinics serving low income, medically underserved populations. Prev Med. 2019 Sep;126:105774. doi: 10.1016/j.ypmed.2019.105774. Epub 2019 Jul 15. PMID: 31319118; PMCID: PMC6904949.
Clinic champions, also found to be more common in Q4 clinics, can play an important role in facilitating EBI implementation.
Sharma KP, Leadbetter S, DeGroff A. Characterizing clinics with differential changes in the screening rate in the Colorectal Cancer Control Program of the Centers for Disease Control and Prevention. Cancer. 2021 Apr 1;127(7):1049-1056. doi: 10.1002/cncr.33325. Epub 2020 Dec 10. PMID: 33301173; PMCID: PMC9242539.
This combined variable indicates that if a clinic directed any additional resources toward a specific EBI, regardless of whether the EBI was already in place or implemented new, then screening rates increased.
Sharma KP, DeGroff A, Maxwell AE, Cole AM, Escoffery NC, Hannon PA. Evidence-Based Interventions and Colorectal Cancer Screening Rates: The Colorectal Cancer Screening Program, 2015-2017. Am J Prev Med. 2021 Sep;61(3):402-409. doi: 10.1016/j.amepre.2021.03.002. Epub 2021 May 14. PMID: 33994253; PMCID: PMC11008572.
Having a clinic CRC screening champion was among the most important program components associated with increased CRC screening both in this analysis and in the earlier analysis.[[10]] The literature supporting the importance of champions in public health program effectiveness continues to grow.[[23]] Champions may be critical to improving CRC screening practice by promoting and prioritizing screening efforts, supporting sustained practice improvements guided by a vision and commitment, and making sure that individual practice changes fit together into a meaningful whole.[[2]]
Sharma KP, DeGroff A, Maxwell AE, Cole AM, Escoffery NC, Hannon PA. Evidence-Based Interventions and Colorectal Cancer Screening Rates: The Colorectal Cancer Screening Program, 2015-2017. Am J Prev Med. 2021 Sep;61(3):402-409. doi: 10.1016/j.amepre.2021.03.002. Epub 2021 May 14. PMID: 33994253; PMCID: PMC11008572.
At the clinic level, a team-based approach was found to support staff ability to integrate implementation of EBIs and supporting activities to promote CRC screening with other patient care activities.
Soloe C, Arena L, Schlueter D, Melillo S, DeGroff A, Tangka F, Hoover S, Subramanian S. Factors that support readiness to implement integrated evidence-based practice to increase cancer screening. Implement Sci Commun. 2022 Oct 6;3(1):106. doi: 10.1186/s43058-022-00347-6. PMID: 36199117; PMCID: PMC9535984.
Third, staff turnover was seen as a major barrier to both implementation success and sustainability. The burden consists of the need to train new staff, the loss of institutional knowledge, and the need to rebuild informal communication channels that are often required for coordination of multilevel interventions and supporting activities.
Subramanian S, Tangka FKL, Hoover S, DeGroff A. Integrated interventions and supporting activities to increase uptake of multiple cancer screenings: conceptual framework, determinants of implementation success, measurement challenges, and research priorities. Implement Sci Commun. 2022 Oct 5;3(1):105. doi: 10.1186/s43058-022-00353-8. PMID: 36199098; PMCID: PMC9532830.
Fifth, the capacity and capabilities of the electronic medical records to support cancer screening by quickly identifying patients due for screening, tracking screening completion, and generating provider-level summary screening uptake were seen as critical for successful implementation and maintenance.
Subramanian S, Tangka FKL, Hoover S, DeGroff A. Integrated interventions and supporting activities to increase uptake of multiple cancer screenings: conceptual framework, determinants of implementation success, measurement challenges, and research priorities. Implement Sci Commun. 2022 Oct 5;3(1):105. doi: 10.1186/s43058-022-00353-8. PMID: 36199098; PMCID: PMC9532830.
To assist public health organizations in correctly implementing EBIs, it is critical to offer intervention-specific guidance in addition to general instructions on how to use evidence as suggested by the Interactive Systems Framework.[[14]]
Escoffery C, Hannon P, Maxwell AE, Vu T, Leeman J, Dwyer A, Mason C, Sowles S, Rice K, Gressard L. Assessment of training and technical assistance needs of Colorectal Cancer Control Program Grantees in the U.S. BMC Public Health. 2015 Jan 31;15:49. doi: 10.1186/s12889-015-1386-1. PMID: 25636329; PMCID: PMC4318175.
Although there is fairly moderate use of EBIs among the grantees, greater adoption and quality implementation of these strategies may be realized through training and individualized TA provided by CDC, other cancer-focused national organizations, and cancer experts.
Escoffery C, Hannon P, Maxwell AE, Vu T, Leeman J, Dwyer A, Mason C, Sowles S, Rice K, Gressard L. Assessment of training and technical assistance needs of Colorectal Cancer Control Program Grantees in the U.S. BMC Public Health. 2015 Jan 31;15:49. doi: 10.1186/s12889-015-1386-1. PMID: 25636329; PMCID: PMC4318175.
Meeting grantees’ training and TA needs is important, as their capacity to implement EBIs will be crucial for meeting the program goal of increasing levels of CRC screening population-wide.
Escoffery C, Hannon P, Maxwell AE, Vu T, Leeman J, Dwyer A, Mason C, Sowles S, Rice K, Gressard L. Assessment of training and technical assistance needs of Colorectal Cancer Control Program Grantees in the U.S. BMC Public Health. 2015 Jan 31;15:49. doi: 10.1186/s12889-015-1386-1. PMID: 25636329; PMCID: PMC4318175.
Individualized TA can provide more in-depth information on how to implement a specific strategy and also address unique contextual factors (e.g., organizational systems such as paper records or electronic medical records, staffing, resources). These combinations of prevention support reported by grantees match the common strategies found in other studies that promote the adoption of EBIs such as in person training and TA,[[29,30]] packaged materials or recommendations, [[31,32]] and conference calls.[[33]] These prevention supports have been proven to increase adoptions of evidence-based prevention strategies.[[31,32,34]]
Escoffery C, Hannon P, Maxwell AE, Vu T, Leeman J, Dwyer A, Mason C, Sowles S, Rice K, Gressard L. Assessment of training and technical assistance needs of Colorectal Cancer Control Program Grantees in the U.S. BMC Public Health. 2015 Jan 31;15:49. doi: 10.1186/s12889-015-1386-1. PMID: 25636329; PMCID: PMC4318175.